You likely woke up with numbness in your fingers or sharp shooting pain down your leg and immediately Googled whether it could get better. That anxiety is understandable. When a nerve stops working, it feels like a vital connection has been severed forever. The short answer to your worry is yes, but the longer answer depends entirely on what kind of injury occurred and how quickly you started treating it. In March 2026, we have more tools than ever before to help nerves heal, but biology still follows its own schedule.
Understanding How Nerve Damage Happens
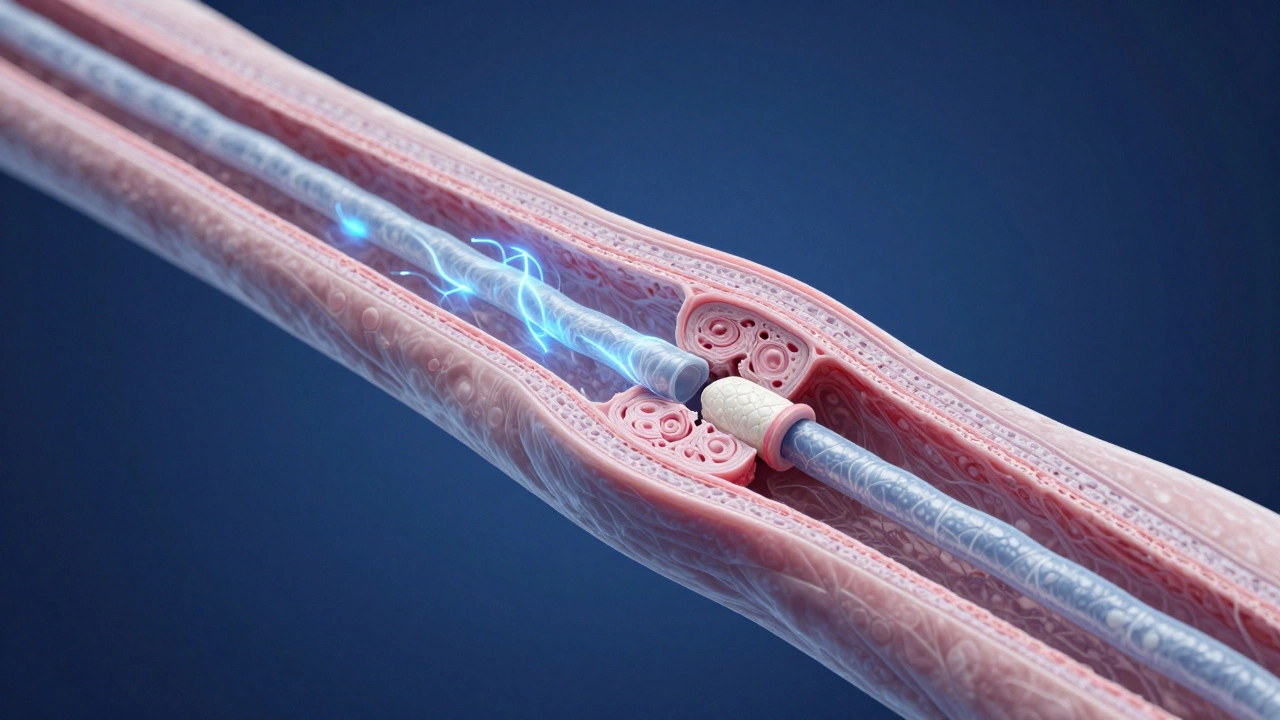
To understand repair, you need to know what broke. Your nervous system is split into two main parts. The brain and spinal cord make up the central nervous system, which doesn’t recover well from injury. The rest are Peripheral Nervesthe long cables that send signals from your spine to your muscles and skin. These are the ones surgeons and rehab therapists focus on when you ask about repairs. When a peripheral nerve gets crushed, stretched, or cut, the electrical signal stops flowing.
The damage usually falls into three categories, known as the Seddon classification. First, there is Neurapraxia, where the nerve is compressed but the structure remains intact. Think of stepping on a garden hose. The water stops temporarily, but once you lift your foot, flow returns. This type heals quickly, often within days or weeks, because the insulation around the wire is just bruised, not broken.
The second type is Axonotmesis. Here, the inner wire is damaged, but the outer casing survives. The nerve fiber degenerates away from the injury site. It takes months for the axon to regrow back down the tunnel to reach the muscle again. With good care, function can return, but the wait is long.
The worst case is Neurotmesis. This means the entire nerve cable is severed. There is no structural continuity left. Without surgical intervention to bridge the gap, the body cannot reconnect the circuit on its own. Scarring prevents regrowth across open gaps in most cases.
The Biology of Regeneration
Unlike brain tissue, your peripheral nerves have a unique ability to regenerate. This process relies heavily on Schwann Cellsspecialized support cells that form the protective sheath around nerve fibers. When an injury occurs, these cells multiply and form a pathway called a Büngner band. The growing tip of the nerve follows this cellular highway back to its original destination.
However, speed matters. A nerve typically grows at a predictable rate of about one millimeter per day. If the injury is ten centimeters away from your hand, that is roughly six months of waiting just for the connection to reach. During this time, the muscle begins to waste away from disuse. If the delay lasts too long, the muscle might die even before the nerve reaches it. This is why timing your consultation is critical.
Diagnosing the Problem Accurately
You cannot fix what you cannot measure. Many people guess they have “just a pinched nerve,” but treatment differs vastly depending on severity. Doctors rely on objective data rather than symptoms alone. One of the most powerful tools is Electrodiagnostic Testinga procedure combining EMG and NCS to map nerve function. Nerve conduction studies check how fast electricity moves along the outside of the nerve, while electromyography checks the electrical activity within the muscle using a small needle.
In addition to electrical tests, modern imaging helps visualize soft tissue. An MRI neurography can show the exact location of a tear or entrapment better than a standard scan. For instance, if you have numbness after a fracture of the forearm, doctors need to know if the median nerve was transected or simply trapped in scar tissue. Misinterpreting this stage often leads to unnecessary surgeries or missed opportunities for recovery.
| Test Type | What It Measures | Best Used For |
|---|---|---|
| Nerve Conduction Study | Speed of signal transmission | Compression issues, carpal tunnel |
| Electromyography (EMG) | Muscle electrical activity | Denervation, muscle wasting |
| MR Neurography | Structural integrity of nerves | Tears, tumors, inflammation |
| Ultrasound | Cross-sectional area of nerve | Guiding injections, locating swelling |
Current Treatment Options in 2026
Treatment strategies depend on the classification mentioned earlier. If you have Neurapraxia, active rest and avoiding compression are often enough. Sometimes medications are prescribed to manage pain, but they do not heal the nerve itself. Over-the-counter options are rarely sufficient for deep neuropathic pain.
For Axonotmesis, the goal is to remove whatever is stopping the growth. This might involve releasing pressure (decompression) so the nerve can heal itself. If scar tissue blocks the path, surgeons perform neurolysis. You need to remember that surgery is not immediate magic. Even after the obstruction is removed, you must wait for the biological regrowth to happen.
In 2026, we also see a rise in regenerative adjunct therapies. While not available everywhere yet, Stem Cell Therapyusing mesenchymal stem cells to encourage nerve healing. Some clinical trials show promising results when combined with surgery to enhance the survival of transplanted nerve tissues. It acts as a fertilizer for the regenerating root.
Surgical Repair Techniques
If the nerve is completely cut, primary repair is the gold standard if done within weeks. Surgeons use microsurgery to stitch the two ends together under high magnification. The alignment of the internal bundles (fascicles) is crucial; mismatching them sends signals to the wrong places. For example, repairing a motor bundle to a sensory bundle creates useless connections.
Sometimes the gap is too wide for direct stitching. In these cases, Nerve Graftingusing a donor nerve from another part of the body to bridge the defect. The sural nerve in the leg is commonly harvested because losing sensation on the side of the foot is less disabling than losing movement in a hand. Synthetic conduits are also gaining popularity, offering a scaffold without taking healthy tissue from elsewhere.
When a nerve cannot reach its target within the lifespan of the muscle, tendon transfers become necessary. Instead of fixing the nerve, the surgeon reroutes a working muscle to do the job of the paralyzed one. It’s a mechanical workaround that restores function even if sensation never fully returns.

The Role of Physical Therapy
Surgery fixes the hardware, but rehab rebuilds the software. Physical Therapyguided exercises designed to maintain joint mobility and retrain the brain. During the long wait for regrowth, joints tend to stiffen. Daily passive stretching keeps the connective tissues supple so the muscle doesn’t contract permanently.
Once the nerve starts firing again, the brain often forgets how to interpret the signals. Sensory retraining helps you distinguish textures, temperature, and pressure again. You might touch different materials with your eyes closed to force the brain to adapt. Without this training, the regenerated nerve might result in hypersensitivity or chronic pain syndromes.
Pain Management Challenges
A common frustration during recovery is that pain can get worse before it gets better. As nerves begin to sprout, they fire erratically. This condition is often called a neuroma. It feels like electric shocks or burning. Topical capsaicin can sometimes help desensitize the area, but prescription medication targeting central sensitization is often required.
It is important to differentiate nerve pain from muscle pain. Muscle pain hurts with exertion and feels like soreness. Nerve pain burns, tingles, or radiates far from the source of injury. Treating muscle pain with ice won’t help nerve pain. You need targeted therapies that calm the overactive nerve endings.
Long-Term Outlook and Expectations
Realistic expectations save patients years of unnecessary suffering. Recovery is measured in months, not weeks. You should expect plateaus where nothing seems to change. These pauses are normal. Consistency is the variable you control. Missing daily exercises slows the timeline significantly.
In cases where full function does not return, adaptation is key. Assistive technology and ergonomic changes can compensate for lost strength. Accepting limitations allows you to move forward rather than dwelling on what you lost. Most patients regain significant quality of life even without 100% return of function.
How long does nerve regeneration take?
Nerve fibers grow approximately one millimeter per day. Depending on the distance from the injury to the target muscle, full regeneration can take several months to over a year.
Can surgery fix nerve damage instantly?
No. Surgery provides the pathway for healing, but the nerve still needs time to biologically regrow down that path to the muscle or skin.
What causes permanent nerve damage?
Permanent damage usually results from complete severance without repair, prolonged crushing injuries, or delays in treatment that cause the receiving muscle to deteriorate irreversibly.
Is physical therapy necessary for nerve healing?
Yes. Therapy maintains joint flexibility during the wait and retrains the brain to process new nerve signals once they arrive.
Does age affect nerve recovery?
Age is a factor. Younger nerves generally have a faster regeneration rate and better plasticity than older nerves, but recovery is still possible later in life.